Zika Virus
The Zika virus is a mosquito-borne flavivirus identified in humans in 1952 in Uganda and the United Republic of Tanzania (1). The Aedes mosquito bites during the day and is the vector that transmits the Zika virus. The most notable population affected by the Zika virus is women who are pregnant, which affects the fetus and causes severe fetal brain defects and neurodevelopmental abnormalities.
(1) World Health Organization. (2018). Zika Virus. Retrieved from https://www.who.int/news-room/fact-sheets/detail/zika-virus
Population, Demographics, Risk Factors
Since November 2015, the Zika virus has been identified in areas such as Puerto Rico, Brazil, and El Salvador. Rates of infection in Puerto Rico have been notable higher among women aged 20-49 allotting to 61% of cases. Comparable laboratory-confirmed cases have been made in Brazil and El Salvador amounting to 75% higher in females then males. Currently, it is not known why the incidence of Zika is higher among women, however, a contributing factor could be related to male-to-female sexual transmission as a possibility.
Central America
Panama has has an increasing trend of cases since the beginning of outbreak. Between late 2015 and early 2016, there was greatest amount of Zika cases in Central America.
Caribbean
The Caribbean countries are showing decreasing trends expect in Anguilla has had an increase in cases.
South America
Paraguay and Peru are the only countries in South America showing an increase in Zika transmission.
Africa
In 2015, 9 cases of Zika-associated microcephaly or CNS manifestations have been reported in Cape Verde, the only country with active Zika transmission.
Southeast Asia
On May 15 2017, the WHO reported 3 confirmed cases of Zika virus in pregnant women in India.
Pacific Islands
Since 2015, active transmission has been identified in American Samoa, Kosrae/Micronesia, Fiji, Marshall Islands, New Caledonia, Palau, Papua New Guinea, Samoa, and Tonga.
Singapore
In August 2016, Zika virus reported 1 Active transmission in Singapore. Since then, Singapore has reported to be clear of active Zika.
United States
In December of 2016, 215 cases have been reported in the United States and 34,463 in U.S. territories.
4,541 cases that have been reported in the United States and 131 in U.S. territories are though travel.
Factors putting you at greater risk of developing the Zika virus include:
Living or traveling to countries where there have been outbreaks increases your risk of contracting the Zika virus. Areas known to have outbreaks include: Islands of the Pacific region, South America, North America, and islands near West Africa.
A person with Zika can transmit the virus to his or her partner through sexual contact. It has been detected that semen, vaginal fluids, menstrual blood, urine, and breast milk can carry the virus. Evidence of sexual transmission of Zika include male-to-female, male-to-male, and female-to-male sex partners. Female-to-female sexual transmission has not yet been reported.
Centers for Disease Control Prevention (CDC) recommends that pregnant couples use protection (female/male condoms) or abstinence, in the event a pregnant woman’s partner had possible exposure to the Zika virus.
Prevalent Health Issues With This Population
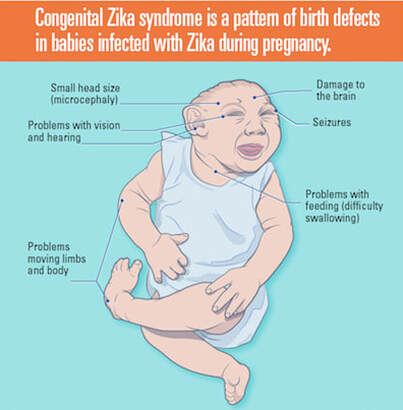
Zika is a virus causing certain birth defects in children and is passed on from mother to fetus. This does not imply that every pregnant woman infected with Zika will have a baby with a birth defect. However, a greater probability of issues increases such as microcephaly, Guillain-Barre Syndrome, and other brain defects.
Microcephaly is a condition where a baby’s head is significantly smaller than the population standards by sex and age. Microcephaly is detected by measuring the head circumference. During pregnancy, the baby’s brain grows along with the head. Microcephaly may arise due to the brain being underdeveloped. During pregnancy or after birth, the brain stopped growing, which results in smaller head size. Microcephaly can be an isolated condition, with no other major birth defects, or it can be linked to other major birth defects. Researchers estimate that about 1 in every 800-5,000 babies is born with Microcephaly in the United States
Related birth defects related to Microcephaly:
Microcephaly is a condition where a baby’s head is significantly smaller than the population standards by sex and age. Microcephaly is detected by measuring the head circumference. During pregnancy, the baby’s brain grows along with the head. Microcephaly may arise due to the brain being underdeveloped. During pregnancy or after birth, the brain stopped growing, which results in smaller head size. Microcephaly can be an isolated condition, with no other major birth defects, or it can be linked to other major birth defects. Researchers estimate that about 1 in every 800-5,000 babies is born with Microcephaly in the United States
Related birth defects related to Microcephaly:
- Seizures
- Developmental delay, such as problems with speech, sitting, standing, and walking
- Intellectual disability
- Complications with movement and balance
- Difficulty swallowing
- Hearing loss
- Vision problems
-
- Guillain-Barre syndrome (GBS) is a rare neurological disorder where the body’s immune system attacks the peripheral nervous system. Weakness and tingling in the body are among the first indicators. Mild cases include a brief weakness, while more severe cases cause paralysis of the entire body. Although there is no known cure for GBS, treatments are available enabling recovery. 60-80% of people are able to walk in six months. However, patients may experience long-lasting effects, such as weakness, numbness and fatigue.
- Based on available evidence, it is assumed that Zika virus infection in a woman who is not pregnant would not pose a risk for birth defects in future pregnancies after the virus has cleared from the blood. Additional infection is not known of. Once a person has been infected with Zika virus, they are likely to have protection from a future Zika infection.
Barriers to Healthcare and Treatment Options for Pregnant Women Affected by Zika Virus

The World Health Organization declared that clusters of birth defects associated with Zika infection during pregnancy constitute a “public health emergency of international concern” (3).
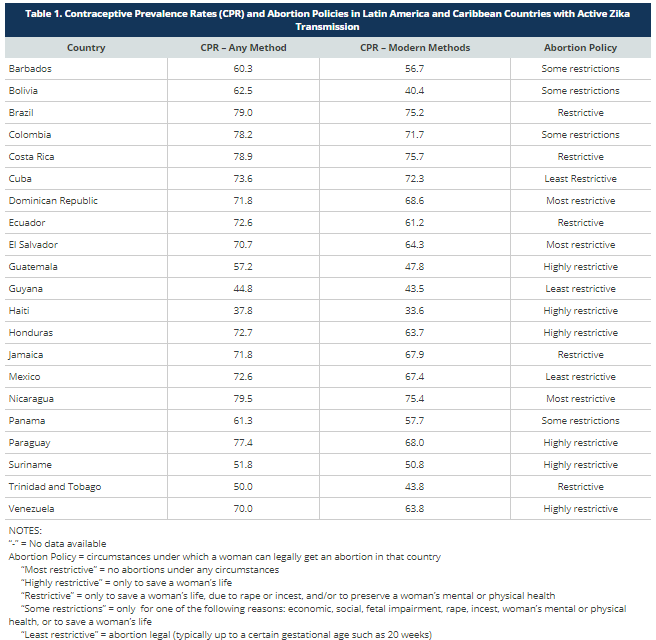
>Public health authorities, such as the Minister of Health of El Salvador, have recommended that women postpone becoming pregnant for a period of time (3). This has raised concerns as women in this region have limited access to contraceptives and other reproductive health services. As the population is 50% Roman Catholic, the use of contraceptives to prevent pregnancies is a delicate issue in this conservative, religious nation (1). In El Salvador, women affected by Zika virus does not have clarity over the laws regarding pregnancy affected by Zika virus (3). Pregnant women in this area are also facing difficulties accessing care as clinics are closed as a result of repeated threats from gangs (1).
>In countries such as Colombia, there is lack of information available regarding the option of using emergency contraception or interrupting the pregnancy legally if infected with the Zika virus (4). As reproductive rights such as abortions are illegal, women are more likely to see unsafe abortions and are putting their health and life at risk (4).
There is no medicine to treat or vaccine to prevent Zika (2).
(1) Ahmed, A. (2018). El Salvador's Advice on Zika Virus: Don't Have Babies. The New York Times. Retrieved from
https://www.nytimes.com/2016/01/26/world/americas/el-salvadors-advice-on-zika-dont-have-babies.html
(2) Centers for Disease Control and Prevention. (2019). Zika Virus – Treatment. Retrieved from
https://www.cdc.gov/zika/symptoms/treatment.html#:~:text=There%20is%20no%20specific%20medicine,www.nytimes.com/2016/01/26/world/americas/el-
salvadors-advice-on-zika-dont-have-babies.htmlGet%20plenty%20of%20rest.
(3)Kates, J. (2016). Zika Virus: The Challenge for Women. Retrieved from: https://www.kff.org/global-health-policy/perspective/zika-virus-the-challenge-for-women/
(4)Morning Edition. (2016). Is it Realistic to Recommend Delaying Pregnancy During Zika Outbreak? Retrieved from
https://www.npr.org/sections/goatsandsoda/2016/01/27/464533090/is-it-realistic-to-recommend-delaying-pregnancy-during-zika-outbreak
>Public health authorities, such as the Minister of Health of El Salvador, have recommended that women postpone becoming pregnant for a period of time (3). This has raised concerns as women in this region have limited access to contraceptives and other reproductive health services. As the population is 50% Roman Catholic, the use of contraceptives to prevent pregnancies is a delicate issue in this conservative, religious nation (1). In El Salvador, women affected by Zika virus does not have clarity over the laws regarding pregnancy affected by Zika virus (3). Pregnant women in this area are also facing difficulties accessing care as clinics are closed as a result of repeated threats from gangs (1).
>In countries such as Colombia, there is lack of information available regarding the option of using emergency contraception or interrupting the pregnancy legally if infected with the Zika virus (4). As reproductive rights such as abortions are illegal, women are more likely to see unsafe abortions and are putting their health and life at risk (4).
There is no medicine to treat or vaccine to prevent Zika (2).
- Treat the symptoms
- Get plenty of rest.
- Drink fluids to prevent dehydration.
- Take medicine such as acetaminophen (Tylenol®) to reduce fever and pain.
- Do not take aspirin and other non-steroidal anti-inflammatory drugs (NSAIDS) until dengue can be ruled out to reduce the risk of bleeding.
- If you are taking medicine for another medical condition, talk to your healthcare provider before taking additional medication
(1) Ahmed, A. (2018). El Salvador's Advice on Zika Virus: Don't Have Babies. The New York Times. Retrieved from
https://www.nytimes.com/2016/01/26/world/americas/el-salvadors-advice-on-zika-dont-have-babies.html
(2) Centers for Disease Control and Prevention. (2019). Zika Virus – Treatment. Retrieved from
https://www.cdc.gov/zika/symptoms/treatment.html#:~:text=There%20is%20no%20specific%20medicine,www.nytimes.com/2016/01/26/world/americas/el-
salvadors-advice-on-zika-dont-have-babies.htmlGet%20plenty%20of%20rest.
(3)Kates, J. (2016). Zika Virus: The Challenge for Women. Retrieved from: https://www.kff.org/global-health-policy/perspective/zika-virus-the-challenge-for-women/
(4)Morning Edition. (2016). Is it Realistic to Recommend Delaying Pregnancy During Zika Outbreak? Retrieved from
https://www.npr.org/sections/goatsandsoda/2016/01/27/464533090/is-it-realistic-to-recommend-delaying-pregnancy-during-zika-outbreak
Key Factors/Social Determinants of Health Contributing to the Overall Health Status of This Population
|
|
Social determinant of health contributing to the overall health status of this population includes poverty. According to Amy Y. Vittor, an assistant professor in medicine at the University of Florida’s Emerging Pathogens Institute, "Lack of running water and waste management, in conjunction with urban crowding and poor housing, has given rise to the perfect set of conditions for the transmission of such mosquito-borne viruses" (2). Poor living conditions in Latin America is notable as window and door screens are uncommon in many locales, and housing often have stagnant tubs or pools of water in dark places that provide breeding grounds for A. aegypti (1). Without any physical barriers, these mosquitos are Access to healthcare is a huge social determinant of health. "These data suggest that women in Latin America and the Caribbean, particularly those who are poorer and live in rural areas and especially those countries with limited contraceptive access and evidence of some contraceptive commodity stock outs may face significant barriers in delaying pregnancy as recommended by some public health authorities, and if they experience an unintended pregnancy or have concerns about being infected with Zika during their pregnancy, have limited options" (3). |
(1) Cohen, J. (2016). So far, Zika is Showing up in the United States Just Where the Modelers Said it Would. Retrieved from https://www.sciencemag.org/news/2016/12/so-far-zika-showing-united-states-just-where-modelers-said-it-would
(2)Healthify Team. (2016). The Zika Virus. Retrieved from https://www.healthify.us/healthify-insights/the-zika-virus
(3) Kates, J., Michaud, J., & Valentine, A. (2016). Zika Virus: The Challenge for Women. Retrieved from https://www.kff.org/global-health-policy/perspective/zika-virus-the-challenge-for-women/
(2)Healthify Team. (2016). The Zika Virus. Retrieved from https://www.healthify.us/healthify-insights/the-zika-virus
(3) Kates, J., Michaud, J., & Valentine, A. (2016). Zika Virus: The Challenge for Women. Retrieved from https://www.kff.org/global-health-policy/perspective/zika-virus-the-challenge-for-women/
Local and Global Policies Regulating the Control and Prevention of Disease in This Population
Due to the severity of the Zika virus and the damaging effects that it has on the fetus, states have set in motion an intensified mosquito control effort.(1) More than likely this requires the use of pesticides sprayed by plane over thick vegetation where mosquitoes are known to breed.(1) The use of aerial pesticides allow for more coverage in a shorter amount of time.
Preparations also involve local, government, and public health care workers to help combat the transmission of the virus. Surveillance systems as well as mosquito traps are also in place to ensure public safety, and gain control over the mosquito population(1). Any mosquitos that are trapped will then be tested to see if they are carriers of the Zika virus.

Given the nature of this virus, and the lack of a vaccine, or medicine to treat it, it is critical that people are well informed about the virus. Public Health workers will work in conjunction with healthcare workers to get accurate reports on how many people have been infected. The CDC has partnered with WHO, and several states to develop a response plan, in the event that a transmission does occur(2).
Since this virus is not limited to just the U.S. the CDC, WHO, and partners, have developed a global policy on their websites to call attention to the devastating consequences of the Zika virus. The infected mosquito is not the only mode of transmission. The global response to Zika is coordinated from WHO headquarters in Geneva (3).
|
SO WHAT DOES THE POLICY ADVISE ? ● Pregnant woman should be cautious as the virus can cause birth defects(1) ● Do not travel to areas suspected of having the disease or outbreaks(1) ● Use precaution or avoid unprotected sex(1) ● Pregnant women should speak with health care provider about risks of Zika infection(1) ● Stay clear of stagnant water(1) ● Wear long sleeves and pants if at all possible(1) ● Using a mosquito bed net(1) ● Using a repellent(1) |
Local and Global Documents Addressing the Needs
STRATEGIC RESPONSE PLAN IN ACTION
Together, the partners developed an improved plan to circulate the importance of the Zika virus.
The 4 main objectives to support national governments and communities in preventing and managing the complications of Zika virus and mitigating the socioeconomic consequences:(3)
● DETECTION(3)
● PREVENTION(3)
● CARE & SUPPORT(3)
● RESEARCH(3)
New efforts in place to reach refugees, people on the move, and those with limited access to information.(3)
DO WE KNOW ENOUGH ABOUT THE VIRUS ?
● The full range of health effects that Zika virus infection during pregnancy is still unknown(1)
● How likely is it that Zika will affect your pregnancy(1)
● Are birth defects definite if you are in fact infected while pregnant(1)
● Not everyone will have symptoms but can still be a carrier(1)
● Can be spread through unprotected sex(1)
● No cure or medication to fight the virus(1)
LOOKING AHEAD
The large outbreak in Americas might seem over, but Zika is and will continue to be a potential risk factor in many countries around the world.(3)
DO YOU WANT TO BE A PART OF SOMETHING BIG ?
Share what you’ve learned about Zika with others. Together we can help raise awareness about this devastating virus.
The large outbreak in Americas might seem over, but Zika is and will continue to be a potential risk factor in many countries around the world.(3)
DO YOU WANT TO BE A PART OF SOMETHING BIG ?
Share what you’ve learned about Zika with others. Together we can help raise awareness about this devastating virus.